 Wirral Surgeon
Excellence for Life
Wirral Surgeon
Excellence for Life
Condition treated
The most important point to remember is that everyone with a bowel problem can be helped and many can be completely cured.
It is never too late to get help with your bowel problems. If you would like some advice on how to approach your GP regarding your bowel problem do get in touch.
Anal fissure
An anal fissure is a painful linear tear or crack in the distal anal canal (back passage).
Anal fissure develop with equal frequency in both sexes; they tend to occur in younger and middle-aged persons.
The exact etiology of anal fissures is unknown, but the initiating factor is thought to be trauma from the passage of a particularly hard or painful bowel movement.
Anal fissure
An anal fissure is a painful linear tear or crack in the distal anal canal (back passage).
Anal fissure develop with equal frequency in both sexes; they tend to occur in younger and middle-aged persons.
The exact etiology of anal fissures is unknown, but the initiating factor is thought to be trauma from the passage of a particularly hard or painful bowel movement.

Clinical presentation
Typically, the patient reports severe pain during a bowel movement, with the pain lasting several minutes to hours afterward. The pain recurs with every bowel movement, and the patient commonly becomes afraid or unwilling to have a bowel movement, leading to a cycle of worsening constipation, harder stools, and more anal pain. Approximately 70% of patients note bright-red blood on the toilet paper or stool. Occasionally, a few drops may fall in the toilet bowl, but significant bleeding does not usually occur with an anal fissure.
Initial therapy for an anal fissure is medical in nature, and more than 80% of acute anal fissures resolve without further therapy.
Management
Failure of medical therapy is an indication for surgical therapy.
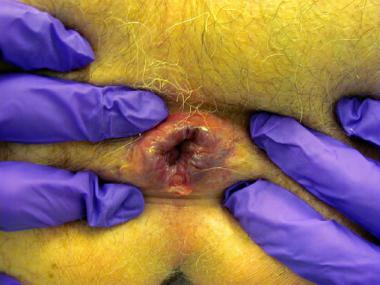

Failure of medical therapy is an indication for surgical therapy.
Lateral internal sphincterotomy is the current surgical procedure of choice for anal fissure; it can be performed with the patient under general or spinal anesthesia. When treating a chronic anal fissure, the surgeon may elect to perform a fissurectomy in conjunction with the lateral sphincterotomy.
Sometimes, long-standing chronic fissures do not heal, even with an adequate sphincterotomy, and an advancement flap must be performed to cover the defect in the mucosa.
The recurrence or non-healing rates for anal fissures after surgical treatment are in the range of 1-6%.